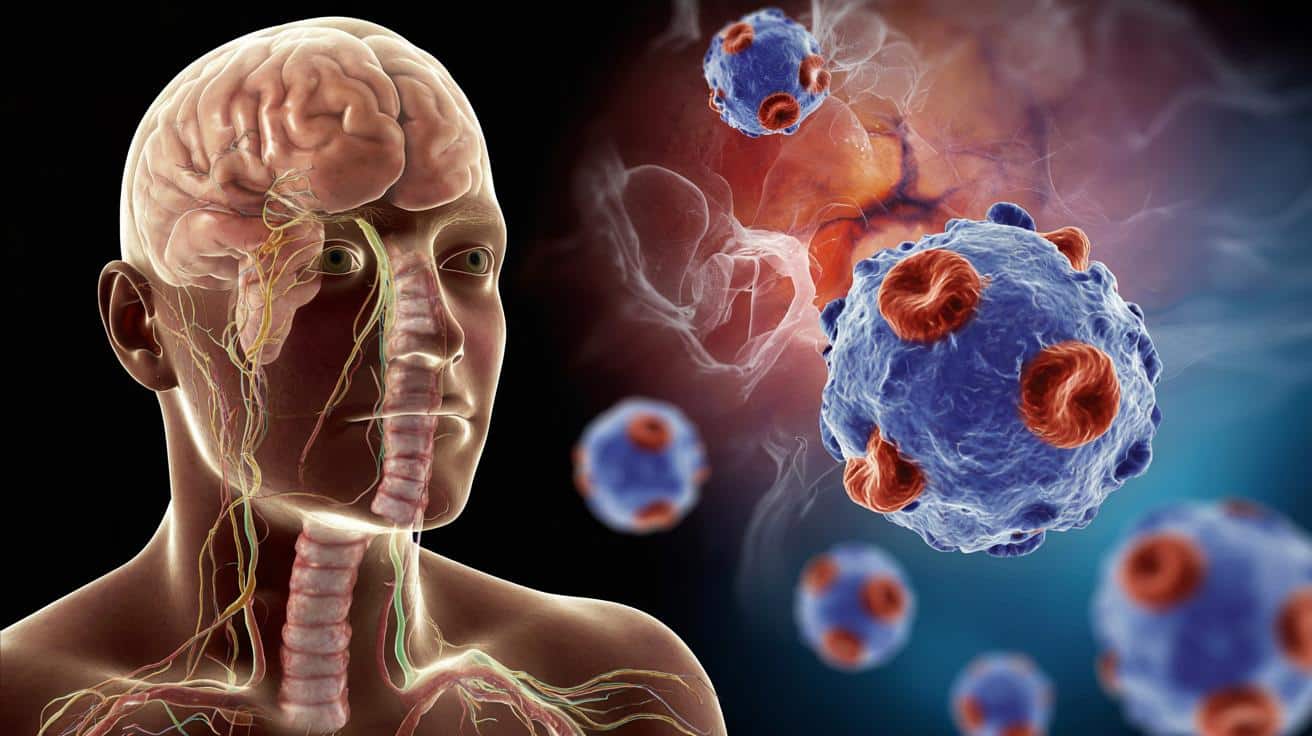
For a small minority, it may help trigger a devastating brain disease.
The Epstein–Barr virus (EBV) sits quietly in most adults, usually forgotten after a teenage bout of glandular fever. Yet a growing body of research suggests this seemingly routine infection may be a key driver behind multiple sclerosis, reshaping how doctors think about one of neurology’s most puzzling conditions.
The quiet virus almost everyone has
By middle age, around 9 out of 10 people worldwide have been infected with EBV. Most catch it in childhood with barely any symptoms. Those infected later, especially in adolescence or early adulthood, are more likely to develop infectious mononucleosis, often called glandular fever.
The virus spreads mainly through saliva. After a short, intense illness with fatigue, fever and sore throat, it withdraws into the body’s B cells, a type of white blood cell. From there, it can remain for decades, usually kept in check by the immune system.
EBV is not a rare or exotic pathogen; it is a near-universal passenger in the human population.
For most people, the story ends there. But EBV has a darker side. It has long been linked to some lymphomas, nasopharyngeal cancer and certain autoimmune conditions. Only in recent years has the strength of the connection with multiple sclerosis become impossible to ignore.
Multiple sclerosis: when the immune system targets the brain
Multiple sclerosis (MS) is a chronic disease in which the immune system attacks the protective myelin sheath surrounding nerve fibres in the brain and spinal cord. This damage disrupts nerve signalling, leading to symptoms that can include visual problems, numbness, weakness, balance difficulties and, in many cases, profound fatigue.
MS typically appears in young adults, with women affected more often than men. The course can be relapsing, with flare-ups and remissions, or progressively worsening. There is no cure, although modern therapies can slow disease activity and reduce relapses.
For decades, doctors have suspected that an infection early in life might help trigger MS in people who are genetically prone to it. EBV has always been a prime suspect, but proof remained elusive.
Evidence for a strong link between EBV and MS
Several large-scale studies over the past few years have sharpened the picture. One landmark analysis of US military personnel followed millions of individuals over time. It showed that the risk of MS soared after EBV infection but did not change after infection with other common viruses.
➡️ 10 hobbies to adopt that help prevent loneliness in old age, according to psychology
➡️ The mental mechanism behind overthinking conversations after they end
➡️ Chia seeds may help the brain regulate appetite and inflammation
➡️ The Norwegian army managed to take control of a bomb dropped by a US fighter jet in mid‑flight
➡️ What it really means when someone walks ahead of you, according to psychology
In people who went on to develop MS, EBV infection almost always came first — sometimes years earlier.
Researchers highlight several key findings:
- Almost every person with MS shows signs of past EBV infection.
- Among initially EBV-negative individuals, those who became infected had a sharply increased risk of later developing MS.
- No other virus studied so far matches this pattern of association.
This does not mean EBV is the sole cause of MS. Genes, vitamin D levels, smoking, childhood obesity and other factors all contribute. Yet EBV appears to be a crucial piece of the puzzle, acting as a trigger in susceptible people.
How EBV might push the immune system off course
Scientists are testing several mechanisms that could explain how a common virus sets off a rare disease. One leading theory is “molecular mimicry”: some EBV proteins resemble components of human myelin. When the immune system responds to the virus, it may accidentally start attacking the body’s own nerve insulation.
Another theory focuses on chronically infected B cells. EBV hides inside these cells, subtly changing their behaviour. These altered B cells might present self-antigens to immune cells in a way that fuels autoimmunity. The success of B-cell–targeting drugs in MS treatment strengthens this idea.
MS may arise when EBV-infected B cells help direct the immune system against the brain and spinal cord.
Researchers also suspect that EBV infection in adolescence, particularly when it causes glandular fever, carries more risk than infection in early childhood. The severity and timing of infection could shape long-term immune responses.
Long-term consequences often underestimated
Because glandular fever is usually self-limiting, its long tail of risk is easy to overlook. Many patients, and even some clinicians, see it as a one-off illness. Yet studies suggest that people with a history of symptomatic EBV infection have higher odds of several later health problems, MS being the most alarming.
The long-term effects go beyond MS. EBV has been linked to:
| Condition | Nature of association |
|---|---|
| Certain lymphomas | Direct viral involvement in tumour cells |
| Nasopharyngeal carcinoma | Stronger link in specific geographic regions |
| Autoimmune diseases | Raised risk seen in some population studies |
| Chronic fatigue syndromes | Suspected role in a subset of patients |
That does not mean EBV inevitably causes these conditions. Most people infected with the virus never develop them. Yet the burden at population level is substantial, because the virus is so widespread.
New therapies and vaccines under intense development
The strengthening link between EBV and MS has shifted research priorities. Several groups and companies are racing to develop vaccines that prevent EBV infection or reduce its impact.
Two main vaccine strategies are gaining attention:
- Preventive vaccines, given before infection, aiming to block the virus from taking hold.
- Therapeutic vaccines, designed for those already infected, aiming to reshape the immune response and limit damage.
Alongside vaccines, experimental therapies seek to directly target EBV-infected B cells. These include advanced antibody-based treatments and cell therapies that train immune cells to recognise and destroy infected targets. Neurologists hope such approaches could one day reduce MS activity or even prevent the disease in high-risk individuals.
For the first time, MS research is seriously considering treatments that go after a suspected root cause, not just the inflammation it leaves behind.
What this means for people with MS today
Current MS treatments already benefit indirectly from insights into EBV. Many of the most effective drugs work by depleting B cells or modulating the immune system, which may limit the influence of EBV persistence.
Doctors do not yet routinely test MS patients for EBV, because almost all would show past infection. Instead, attention is turning to how early in life future generations might receive EBV vaccination and what that could do to MS rates decades later.
Key terms patients keep asking about
For readers trying to piece this together, a few concepts often cause confusion.
- Latency: After the initial infection, EBV enters a dormant state inside B cells. The virus is not gone; it is just quiet.
- Autoimmunity: The immune system usually distinguishes self from non-self. In autoimmune diseases like MS, that distinction breaks down and the body’s own tissues are targeted.
- Relapse: In relapsing–remitting MS, symptoms flare for days or weeks, then partially or completely improve before the next episode.
People sometimes assume “having EBV” means being contagious for life. In reality, viral shedding in saliva fluctuates. Periods of higher shedding can occur without any symptoms at all, which explains the virus’s near-universal spread.
Everyday scenarios and risk perspectives
Consider two teenagers. One catches EBV at 14 and spends weeks exhausted with classic glandular fever. The other is infected unnoticed at age three. Both will carry the virus for life. Epidemiological data suggest the first teenager, with late, symptomatic infection, may have a slightly higher lifetime risk of MS than the second. Yet for both, the absolute risk of MS remains relatively low.
This kind of scenario helps frame the debate: EBV is a necessary step in many MS cases, but by itself it is not enough. Genes, environmental exposures and lifestyle all feed into whether the illness ever appears. That is why public health experts are cautious about overpromising what an EBV vaccine might achieve, even as expectations for meaningful risk reduction remain high.
For most people, EBV will stay a silent passenger; for a few, it is one of several hits that push the nervous system past a tipping point.
For individuals already living with MS, these findings bring mixed feelings. On one hand, they suggest that past infection, not personal choices, played a major role. On the other, they open realistic hope that the next generation might face a lower risk, thanks to vaccines and virus-targeted therapies now moving through trials.